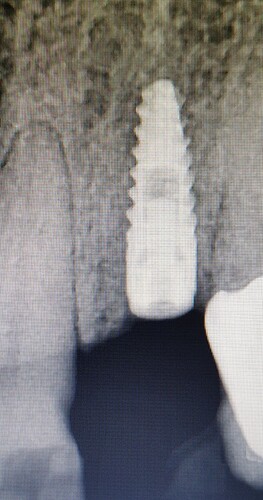
I was placing biohorizons 3.4 x 10.5mm implant at lateral upper incisor with small fenestration at apico-buccal side, after usual drilling i put the implant, when i tighten the cover screw i can feel the implant spinning, i wont use bigger diameter implant because it can make the fenestration even bigger, so since i cant remove the cover screw again, i push down the implant lightly and torque it clockwise with hand driver until i feel its stop spinning and i cant rotate it again with my finger, after that i put the bone graft and membrane like you all usually do and get a good closure, what do you think about the spinning implant? Will it ossteointegrate?
Looks like there was no mobility- so Yes! It will osseointegrate. I would open & place healing collar after 3 months.
Hi. In all likelihood, it will integrate provided that soft tissue in-growth does not occur. But we know from the literature and experience that better primary stability will lead to more predictable integration. In this specific case, since there appears to be much more bone apical
To the implant, I would have removed the spinner and reprepped and placed a longer implant to obtain primary stability. Of course, my opinion is limited considering I’m only looking at a 2D radiograph and no clinical presentation.
Let us know how this case goes.
it will be good ,don’t worry.
Just like everyone else has said it will be fine. As far as primary stability as determined by insertion torque let’s not forget that there are many successful press fit implant fixtures out there and by the nature of the press fit design I can assure you they were “spinning” at the time of insertion. Unless I plan to load a fixture I pay very little attention to insertion torque… IMHO primary stability as determined by insertion torque is highly overrated and obsessed over.
This should turn out fine. That last bit of engagement helps alot. Using a longer implant could have helped. I presume from you primary closure comment that you buried it. Good work!
@prndds since this is designed to be a forum in which clinicians can discuss and learn I was wondering if you could clear up a statement from your last post. You said that it “looks like there was no mobility” and I was hoping you could explain just how from the radiograph and information provided you were able to visualize an absence of mobility. I would assume that the spinning of the implant would be considered mobility though I can’t tell from the image if it is spinning or not but just like you said and I agree that it will be fine. Because the individual did post that he hand tightened the fixture until it stopped spinning freely at that point I would have opted to go ahead and place a transmucossal healing collar if it were not going to interfere with the patients esthetic demands. I am probably a little different when it comes to submerging a fixture because I trained with Straumann/ITI tissue level fixtures and with a 1.8-2.8mm transmucossal collar we were forced to immediately expose a lot of “unstable” fresh fixtures and what I discovered is that they worked great.
Can you explain how “expose unstable fixture can ended work great?”
At last i think i can hv good night sleep
Im not sure how many torque on that implant, but i cant rotate it more with my finger
@duvalie to clarify what I meant. The straumann tissue level fixture has a 1.8-2.8mm transmuccosal collar and when using it you can not submerge or cover it like we can a bone level fixture. What was meant by the statement is that even in cases of poor stability we were forced to leave these fixtures exposed with what amounts to a healing abutment. Low and behold they experienced the same overall survival rate as submerged bone level fixtures. People can draw a number of conclusions from this but the one that I took away is that primary stability as measured by insertion torque is a minor factor despite the hype within the industry. I have placed at least 100-200 fixtures over the years that lacked what most would consider adequate primary stability because the were “spinning”. As a result of my past experience utilizing tissue level fixtures I have confidently exposed these, unstable by today’s implantologist definition, fixtures via a healing abutment placed day of surgery and the end result is fine. I hope this helps clarify and possibly offer a different perspective on primary stability…
Thanks for the explanations doc, i hope one day i can afford straumann system
@duvalie as someone who has utilized many different implant systems over the past 20 years I finally settled on Zimmer about 7-8 years ago and now use it exclusively. I have used and have kits still in my office for Biomet 3i, Straumann, Bio Horizons, Blue Sky Bio, Implant Direct, Ditron, Nobel Biocare and Zimmer. After using each one of these systems I can say that they all have performed well except for Bio Horizons. I will go on record and say that they all work except that I have seen nothing but problems, both with the fixtures that I placed as well as the many from other offices that find there way to me, with Bio Horizons. The long term soft tissue response with this system is absolutely horrible and I can only assume that it has to do with their Laser Lock gimmick. I have gone away from offering advice as it is rarely appreciated and resorted to offering suggestions instead. I would suggest that you pay attention to how these fixtures respond and possibly start looking into an alternative system. I would like to stress that this is something that I along with a slew of other like minded periodontists have concluded and while I know Bio Horizons markets heavily and sells a ton of stuff their booth at the last Southern Academy of Perio was a ghost town… I think experienced clinicians are realizing something about this flawed system.
If you guys remember this case, today (about 4 month after implant placement) i placed the healing abutment, and it looks good, no mobility, no spinning, no pain, hope it can serve well
Interesting. I have placed 5000 implants in my career over the last 26 years. 3000 of them were Biohorizons along with a variety of others. My success rate across the board has been pretty much the same. I think it comes down to whatever system you are comfortable with and have learned the intricacies of that system. I can’t think of a system where we had more that 4-6% failures, which is current with the literature.