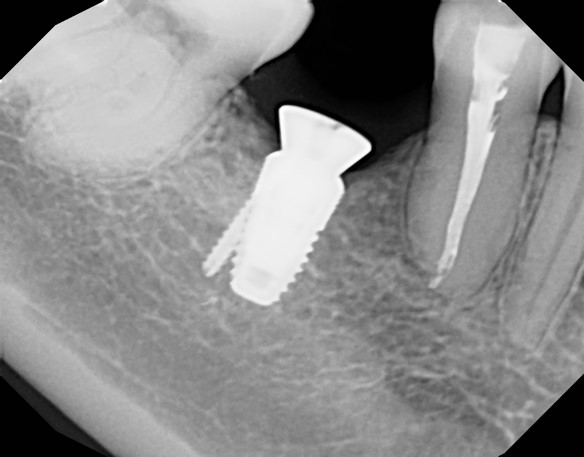
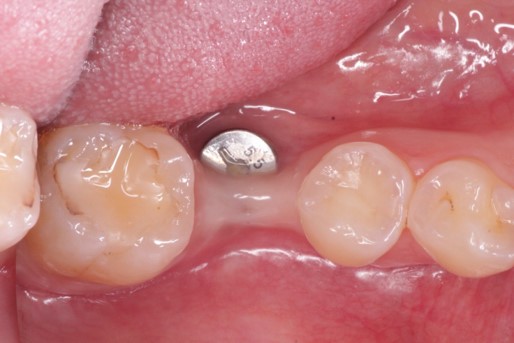
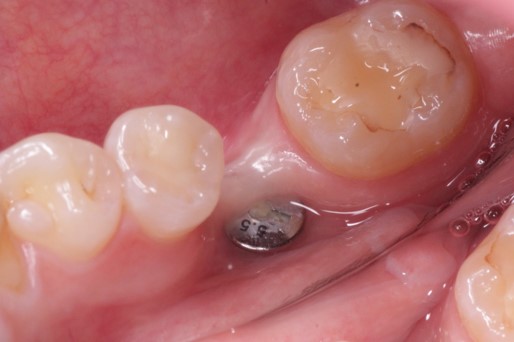
This 45 year old female presented to have implant #30 restored. She is aware that its position leaves a lot to be desired but she will not consider removing the implant and replacement. There is an obvious mucogingival deformity that you would like to address. What plan would you propose to provide an adequate zone of keratinized tissue on both the buccal and lingual of the implant prior to restoring it?
timcarter comments:
I would harvest a thick CT graft and utilize the healing abutment as a "tack" to stabilize it on the buccal and lingual. If possible get a slightly taller healing abutment and cut a small slit in the center of the CT graft. Make a crestal incision and pop the graft over the healing abutment to allow it to drape over the buccal and palatal and place 2-3 simple interrupted gut sutures. After 3-4 weeks you should have a thick band to protect the bone in the future.
drdangober comments:
Interesting approach. Can you explain how you would actually perform the recipient prep if you were to do this?
timcarter comments:
Actually I don't think the recipient preparation is all that important but I would just make a crestal incision #29-31 to expose the top of the fixture as well as the buccal/lingual bone. Similar to the case you posted a while back where you cut a hole in a membrane and popped it over the top of a healing abutment I would do the same with a CT graft. The only reason I mentioned a taller healing abutment is because the thick graft will want to ride up while you are securing it so it just makes it easier. I would then suture the buccal and lingual flaps over the graft. Most likely it will result in a thick covering of CT which can be shaped with a contoured healing abutment prior to impression/restoration. The goal is to get too much tissue and hopefully have to trim some away.
ninjadds1227 comments:
Can we see a cbct Criss section image? Where is the broken mini implant buccal lingually and does it touch the implant? Even with an angled abutment this will likely hurt her tongue after restoration. So before you plan soft tissue- what’s going on with the implant and broken implant. This may be better served burying and doing a bridge as you will be on the hook when she has issues swallowing due to a sore tongue- so document really well.
drdangober comments:
Thanks for highlighting the potential tongue problem- that's definitely important to make the patient aware of and the bridge option should def be discussed. Can you explain why you see the need to know more about the broken screw? It appears to have been like that for a while and the implant's bone presentation is def consistent with the implant.
ninjadds1227 comments:
The broken mini implant may be fully within the bone and not touching the implant but without a cbct you can’t know. The fractured mini- implant could perforate the buccal or lingual and become a wick for bacteria. Without all the information you can’t simply ignore it. It also highlights that the patient may have chosen this treatment due to cost -and it may further give you insight as to who placed the implant, why it wasn’t done with respect to prosthetic crown planking and whether the patient put constraints on her care or if it was a dentist that didn’t properly evaluate the patients needs and for e factors. You need to understand thenoatienr and the case before you jump in- just my opinion.
timcarter comments:
That broken screw doesn't mean anything other than some benign object is stuck there... I agree with you it is no big deal.
timcarter comments:
I would like to speculate for a moment... Dr. Gober is a periodontist and as such it is generally frowned upon for us to criticize the work of others. I understand that in the general dentistry and specifically that of the Super Dentist world it is relatively common to advertise superiority over another clinician and to more freely criticize other treatment. That is more acceptable as you are maintaining control of all treatment and do not rely on other clinicians to feed you business. The only reason to explore the rabbit hole of the origin of the broken screw would be to shame another provider and in this case it could very well be that the doctor that did this is now humbled and more likely to become a future referral. How can this broken screw act as a bacterial wick if healthy soft tissue is sealing it???
ninjadds1227 comments:
I find this to be a very negative response. There was nothing in my response that wasn’t based in factual implant dental explanation.
A broken implant is not a matter of shame but a fact.
Wicking can occur if the broken implant fenestrated the buccal or lingual plate. Also there can be galvanic reaction to dissimilar materials. You don’t know if the broken screw is a titanium alloy or not. You don’t know if it touches the other implant. Either way this is vital information for anyone wishing to restore this case. Lastly the implant is in the wrong place! I really don’t care if someone is a Periodontist, oral surgeon or highly trained GP, the implant placement needs to be prosthetically driven!
Next, if you place a new implant in a site with a broken root, implant or foreign body, you need to locate it in 3 dimensions and ascertain if it may interfere with your outcome. He who touches the case last owns it.
Your assertions about criticizing anyone are wrong and specious.
Read what I wrote! This is lingually placed and we cannot judge if it even can be restored without also seeing the cbct. It will create a problem with the patients swallowing and if a screw retained abutment can save the case that’s great. It will still have a hidden cantilever to the buccal as it’s too far to the lingual. Read my answer as a sincere query without judgement and you may actually agree with what I have written.
Sincerely and without judgement,
Richard Winter DDS MAGD DABOI FAAID DICOI
timcarter comments:
I agree with you and my apologies for the misunderstanding. To be clear I was relating to Dr. Gober's position. As a fellow periodontist that did not place the fixture nor will I be restoring it I do not give a da%* about the broken screw. The patient was referred to address the mucogingival condition around a fixture that another legally credentialed dentist (possibly a good referral) has decided requires augmentation prior to restoration. That is all of the information needed for Dr. Gober and/or myself to perform our requested service.
alan comments:
It is grossly malpositioned
Remember one thing when you are preparing to restore this case
"The last person who touches it, owns it ."
Just ask yourself one question:
Why put yourself in this predicament ?
drdangober comments:
Very good point in terms of managing success and personal stress! In this particular situation, I am not the one who is actually restoring this- I was called in to analyze the soft tissue issue.
timcarter comments:
Far from perfect but I disagree that this fixture is grossly malpositioned. If you evaluate the tooth position of a typical mandibular arch you should notice that the height of contour of a mandibular first molar is typically quite lingual to that of the second premolar and often even the second molar. While this appears to be placed well to the lingual it is most likely an illusion because of the buccal concavity which will be addressed with the soft tissue graft. Yes it is placed to the lingual but I do not believe it to be as bad as some may propose and I think it is a relatively simple fix and easily restorable.
mb60 comments:
Many variables exist… move the molars distal, have perio split the flap with an intracrestal incision , remove the healing abutment, place cover screw, l-prf membranes (or mucoderm ? Or Synosis) and cover the ridge both buccal and beyond the lingual soft tissue button hole defect and suture carefully with 6-0 gortex or nylon . May need a second phase gingival surgery as well. But should be restorable
drdangober comments:
That sounds like a lot of work! The soft tissue graft substitutes don't accomplish much in terms of gingival gain. I personally don't see how the tissue can be managed surgically the way it is. I like your idea of removing the healing cap and placing a cover screw. I was thinking to do that to allow the soft tissue to completely cover the implant, then make an incision just buccal to the gingiva and push it lingual and perform a free gingival graft on the buccal.
removing the HA and placing a cover screw may close the opening and allow a gingival emergence. I would do that, wait 4 months, and when uncovering it, have the patient ready for a FGG if needed.
I have virtually eliminated post op pain complaints from FGG donor sites. We premake a vacuform splint to cover the wound and also suture L-PRF membrane to the donor site. The more they wear the splint (esp w eating) the longer the PRF releases Growth Factors…up to 14 days.
Good luck


