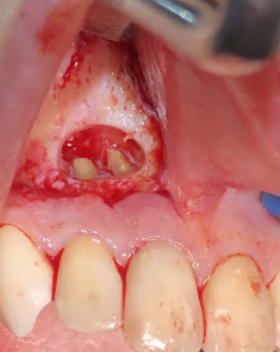
This is just a picture from the internet. I was wondering if this kind of flap may decrease the blood supply of the gingival tissue coronal to the incision line? Is it against the principle of flap design? Is it a normal or recommended flap design for apicoectomies? I also assume it is hard to suture to the stable attached mucosa. Or do you prefer to make the incision for apicoectomies apical to the bony defect?
K Gilani comments:
This seems the right incision for apicoectomy. It should be placed in a semilunar fashion with the convex side toward the teeth. And no blood supply is not compromised. You can suture by mobilising the flap margins. Suture shouldn't be placed in the defects.
DrT comments:
Suturing to attached keratinized tissue is a good thing
Tim Carter comments:
This is the "Norm" in Endo and I recall arguing with the Endo residents about such back when I was doing my perio training alongside them. While it is perfectly OK for this patient in this photo, it should be avoided in cases with pigmented gingiva as it will produce a scar. The other problem with this design it that it requires some experience to handle a flap of pure mucossa without tearing it and it is taught to novice endo residents because that is "the technique" in all of their texts. While it is just my opinion I would prefer a wide sulcular incision with a vertical release distal to the canine as it allows for much easier flap management and less pulling an tugging on the weak tissue. Since this photo probably came from an endo site I assume that they probably closed it with silk suture and had the patient back in 3-4 days to remove suture because again that it "the technique". I rarely, if ever, use anything other than Chromic Gut suture because my experience has also shown me that patients generally dont like having sutures removed from inflamed mucossa and I have yet to come across any perio/implant surgery that cant be closed with resorbable Chromic Gut!!!
Greg Kammeyer comments:
Yes this is a common flap design for an apico. It usually is semilunar which as Time points out puts less pressure on the flap margins. It does compromise blood flow yet I'm not aware of a study that shows that is an issue. I would prefer this flap for that surgery over a sulcular incision to avoid altering papilla height. Certainly how much this area shows in the patients smile affects which incision method used. I would favor gut here and use monofilament suture when advancing flaps for bone regeneration. When suturing mucosa, the gut is especially nice at Tim pointed out for patient comfort and the trick when suturing mucosa is to not put too much tightness in the suture which keeps it from forming an unsightly scar.
Mark Barr comments:
First of all- Tim, why slam “the endodontists”? Too funny. Any incision compromises blood suppy, the question is- will it slough? Some of the questions we should ask ourselves before we incise are. Where are the danger zones? Can I suture that closed? Where will the tie end? How much recession will follow? Etc…
The flap should be as long as is needed to fix the problem as quickly as possible without being careless. Flaps heal side by side and not end to end…
Before suturing irrigate the depths of the flap well with sterile saline, re-position the tissues well and compress to decrease “dead spaces”. Than suture with the material that serves the wound and not the clinicians schedule. The above surgical picture is ridiculously poorly performed. The flap is under way to much tension. The bone is being over zealously dried. These two errors will cause more harm than good. The semi-lunar incision, which this is not, is fine for the Apico-ectomy. And always perform a retrofill when doing an apico; curettage only is insufficient on old endo. As clinicians we must be careful of what, where and how we learn our protocols and who we choose to learn from.
Scott Bobbitt comments:
This is a standard Leubke-Oschenbein flap—perfect for apical access when you don’t want to disturb the periodontal marginal tissues like would happen with a “standard” intrasulcular incision. Only drawback is the potential for scar formation if the incision isn’t beveled and the wound edges reapproximated carefully.
guest comments:
No one's gonna see a scar in the mouth?? Do you worry about a scar or the product of the operation? It's like a pregnant woman having a visible C-section scar (after the delivery)? Who really cares about a scar? I'd worry about a healthy delivery of a baby than a big ol scar. Here, do you worry about successful apicoectomies .............or a noticeable "visible" scar (after the procedure)?
Stoler, Kenneth comments:
In my experience, semilunar incisions heal with a puckering effect and leave a scar. I abandoned them. Straight line incisions heal extremely well with minimum scarring.
Matt Helm DDS comments:
Let's face it: oral surgery is as much an art as it is a science. And what this photo shows is certainly no art -- on the contrary. Two of the best OS's I ever knew, early on, used to say that "you can do a lot of wrongs and it will heal, as long as you don't over-abuse the tissues, remember the basics, and don't cut like a cowboy". They were right. If you saw their hands, they used to operate more like they were playing a fine musical instrument -- never rough, every move calculated. Who you learn from is paramount. This photo shows a flap that is poorly designed and is terribly overstretched, as well as a defect that has been excessively washed and dried, possibly compromising post-op blood supply. I always prefer to use a beveled semilunar incision (the bevel insures adequate blood supply), as it doesn't cause recession like a sulcular incision does. In my view, a sulcular incision is excessive, and raises not only the specter of gingival retraction and possible alteration of the interdental papilla (both undesirable in the anterior area) but, also unnecessarily destroys the cervical periodontal ligament, accelerating the onset of perio pockets. The suture should always be placed over bone, not over the defect. Gently repositioning the flap, gently depressing it to eliminate voids and ensure proper seating, and suturing without tension with equal distance between the sutures are also key. If these basics are followed, choice of suture becomes almost irrelevant. One other trick I use is to place in the sulcus a cotton roll around which I've wrapped a little iodine gauze as a last step, post-suturing. It's a very old technique that keeps light pressure on the area, thereby preventing excessive local swelling, while the iodine gauze minimizes infection risk in the initially crucial first 24 hours. It also serves as a "patient control" tool for the first crucial 24 hours post-op, "reminding" the patient they had surgery and preventing harmful actions like rinsing or brushing. Additionally, a smoker can smoke in this way. (Don't ever think that a die-hard smoker won't smoke simply because you instructed him not to. The best thing you can do for such a patient is to teach him/her how to smoke without causing harm.) Suture removal at 5-7 days thus becomes easy and routine, with no inflammation present. I've done an inordinate number of apicos following these tenets, and of course always placing a retrograde filling, and never had a failure, despite some claiming that 50% of apicos fail. Many years ago, I once rebuilt the whole distal half of an upper canine root in amalgam, and did it through a semilunar incision, which goes to show that you don't need some G-d-awful large flap. (An implant or another bridge were not alternatives due to patient's extreme financial constraints. When initially told that the root was compromised and should be extracted, the poor woman, who also had 3 kids, started crying profusely at the prospect of losing her anterior bridge.) I had discovered intra-operatively that the whole distal half of the canine root had decayed due to a long-standing RCT perf. It worked perfectly, and the tooth -- which was one of two supporting abutments of an anterior bridge (the other abutment being the other canine) -- lasted another 15 years! Now THAT is art! (if I do say so myself) :sunglasses:
