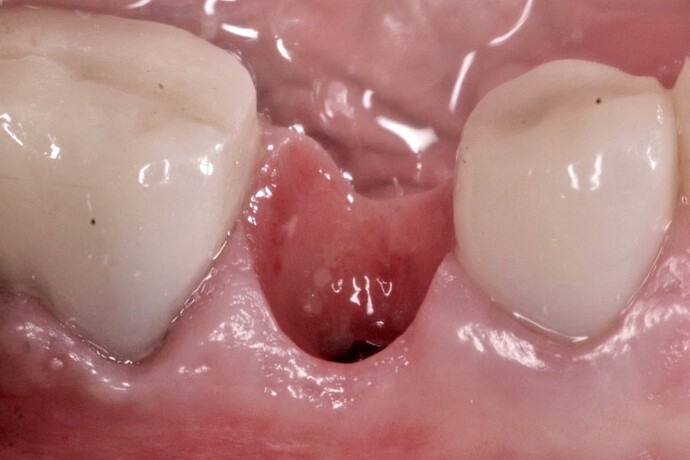
This video case demonstrates the use of a DALI amnion-chorion membrane in combination with a porcine collagen membrane for guided bone regeneration in a previously failed implant and graft site.
The Amnion-Chorion Membrane has shown promise for several clinical applications in dentistry, including tissue regeneration. This is not surprising as Amnion-Chorion Membranes have been used successfully in other medical fields for many years, including ophthalmology, which seems to provide a good comparison for dentistry, given that the oral cavity and eye share several common properties. 1
The beneficial effects of Amnion-Chorion Membranes (ACM) have been documented in several studies. 1. As regards to tissue regeneration, the fact that ACMs provide intrinsic growth factors is especially interesting considering the role growth factors play in enhanced healing. Despite the potentially positive outcomes from using an ACMs, we think clinicians have been slow to adopt these membranes because of the unfamiliarity with the handling of these membranes, and perhaps more importantly a lack of clarity on the specific indications for these membranes.
We believe that an excellent application of ACMs is in a dual-layered membrane technique, where the ACM is used in conjunction with a collagen membrane. 2,3,4 The enhanced healing provided by the ACM is especially useful in previously failed cases or where other factors suggest potentially challenging regenerative outcomes for GBR. The efficacy of the dual, or double, layered membrane technique is well-documented. 2 Usually it is suggested to use 2 collagen membranes or a collagen membrane + PTFE membrane. However, we think an Amnion-Chorion Membrane is the perfect choice for a secondary membrane layer, due to the many beneficial properties of the ACM.
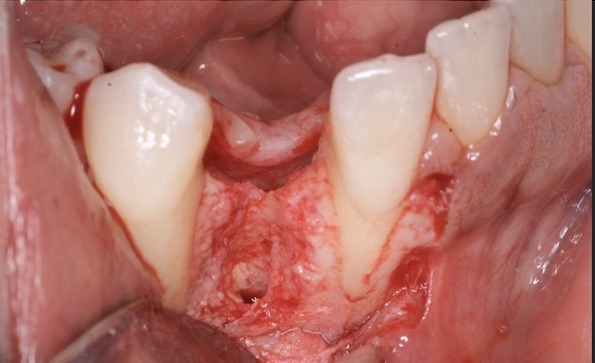
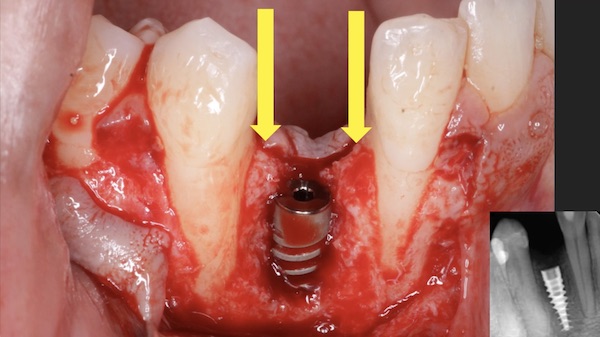
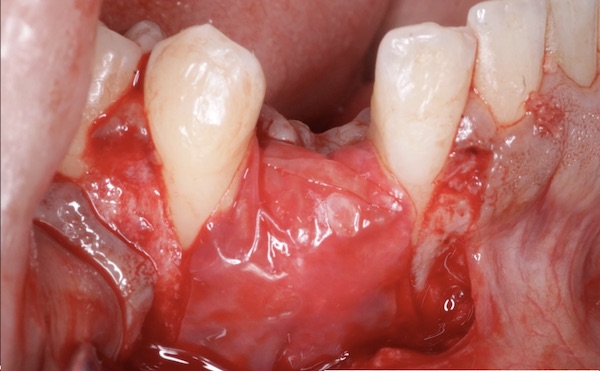
In the case shown in this video, a patient was referred to the office following a failed implant from another surgeon. The referring office removed the implant and grafted the site. Unfortunately, after re-entering the site it was clear that the graft had failed. The site was subsequently cleaned out, and a new implant was placed. Even though, the site obviously still needed substantial regeneration, we were confident in GBR because of the nice bone peaks on the adjacent teeth, and that fact that the new implant was placed well within the alveolar housing.
The specific GBR procedure was follows:
-
An OsseoSeal collagen membrane, was first tucked under the lingual flap.
-
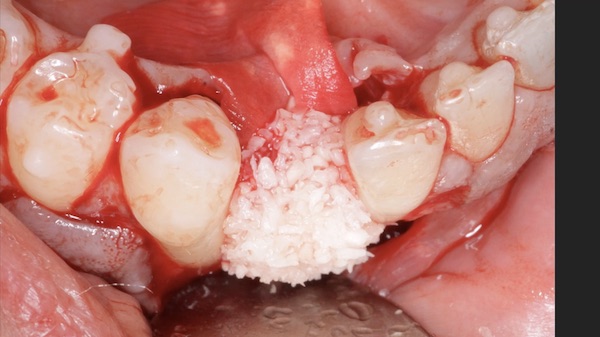
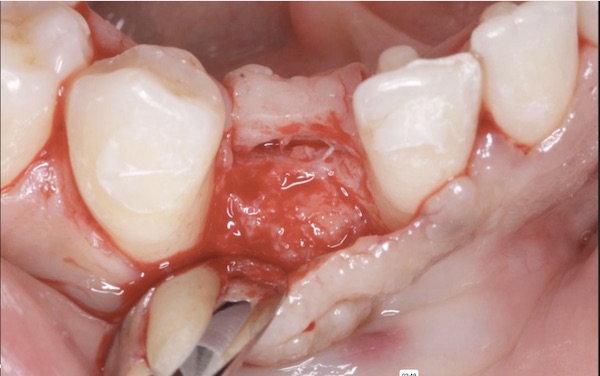
DALI Mineralized Cortical Cancellous Bone Mix, was then added at the top of and around the implant.
-
The OsseoSeal membrane was then placed over the graft, extending onto native bone
-
A DALI Amnion / Chorion Membrane was layered on top of the OsseoSeal Membrane for enhanced healing.
![]() It’s important to remember that ACM’s are extremely difficult to handle once they get wet. So please be sure to handle and manipulate the membrane when it is dry.
It’s important to remember that ACM’s are extremely difficult to handle once they get wet. So please be sure to handle and manipulate the membrane when it is dry.
- Primary closure was achieved following specific suturing techniques (see Suturing for Tension-Free Primary Wound Closure).
![]() While the literature suggests that ACM can be used without primary closure, from our experience the membrane seems to perform better when NOT exposed.
While the literature suggests that ACM can be used without primary closure, from our experience the membrane seems to perform better when NOT exposed.
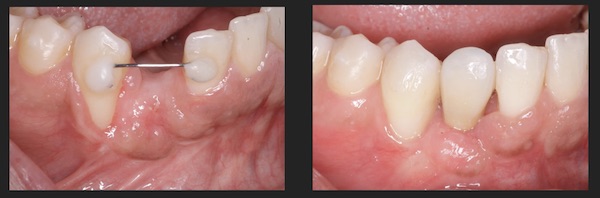
At 3 Months follow up, the site was re-opened. There was excellent soft issue healing, and an increase in ridge contour. Furthermore, the implant was well integrated and overall the GBR procedure was successful. Interestingly, some root coverage was achieved as well following the GBR, which we think could possibly be attributed to the use of the Amnion Chorion Membrane.

References
- Front. Bioeng. Biotechnol., 10 June 2021 Sec. Regenerative Medicine Volume 9 - 2021. Surgical Application of Human Amniotic Membrane and Amnion-Chorion Membrane in the Oral Cavity and Efficacy Evaluation: Corollary With Ophthalmological and Wound Healing Experiences Stéphane Odet et al.
To date, ophthalmology is one of the most popular applications of hAM in routine use. The tissue is used as a graft, spread onto the ocular surface to treat epithelial defects or ulcers, or as a bandage to cover the ocular surface to promote healing. Since the mid-1990s, there has been a growing interest in using hAM for oral surgery to accelerate tissue regeneration. Chorion and amnion-chorion membrane (ACM) products are also very popular in this indication because they provide not only better handling and thickness, but also provide intrinsic growth factors…Because Amnion Membrane (hAM) does not have any space maintenance capabilities, some authors suggested using multiple hAM layers and reported its usefulness as a barrier. Two layers of hAM can be folded over bone allograft, delaying its degradation or enhancing its barrier function without any consequences.
- Clin Oral Implants Res. 2009 Oct;20(10):1124-32. The efficacy of a double-layer collagen membrane technique for overlaying block grafts in a rabbit calvarium model Su-Hwan Kim 1, Do-Young Kim, Kyoung-Hwa Kim, Young Ku, In-Chul Rhyu, Yong-Moo Lee
Furthermore, the double-layer technique using non-cross-linked collagen membranes (BioGide((R))) can enhance the efficacy of the onlay block bone graft technique.
- J Periodontal Implant Sci. 2011 Oct; 41(5): 253–258. Secondary closure of an extraction socket using the double-membrane guided bone regeneration technique with immediate implant placement Jeong-Ho Yun,corresponding author Choong Man Jun, Nam-Sik Oh.
This last issue is addressed herein using the double-membrane (collagen membrane+high-density polytetrafluoroethylene [dPTFE] membrane) technique…Secondary closure of the extraction socket and immediate guided bone regeneration using the double-membrane technique may produce a good clinical outcome after immediate placement of a dental implant in the posterior area.
- Compend Contin Educ Dent . 2022 May;43(5):E1-E4. Use of a Sugar-Crosslinked Collagen Membrane in Conjunction With a Dehydrated Amnion/Chorion Membrane for Guided Bone Regeneration Around Immediate Implants Matthew J Fien et al.
The use of a collagen membrane in combination with a dehydrated amnion/chorion membrane (dHACM) can facilitate stabilization of the bone graft and membrane by providing the benefits of a long-lasting bioabsorbable collagen membrane in addition to the unique benefits of an amnion/chorion membrane.