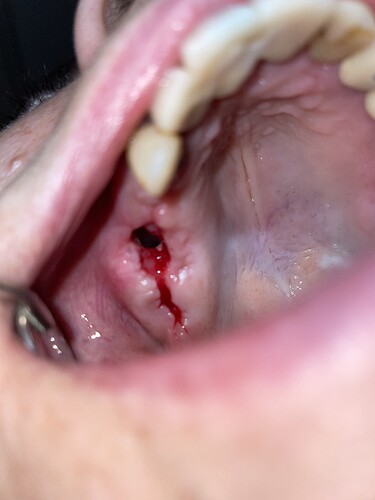
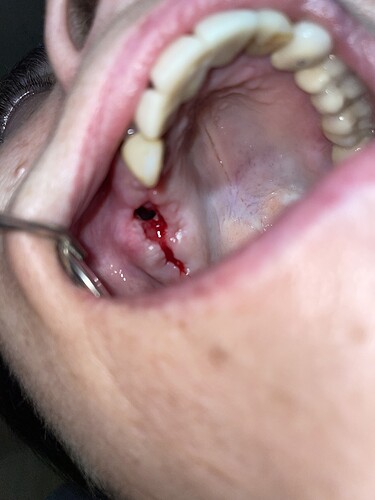
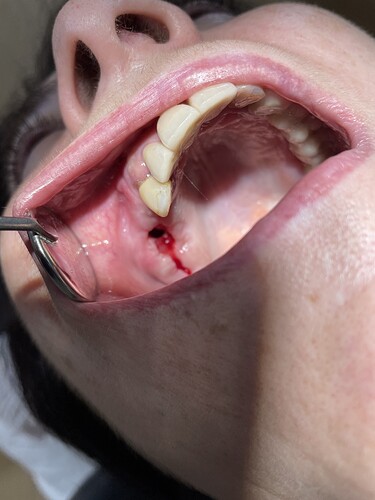
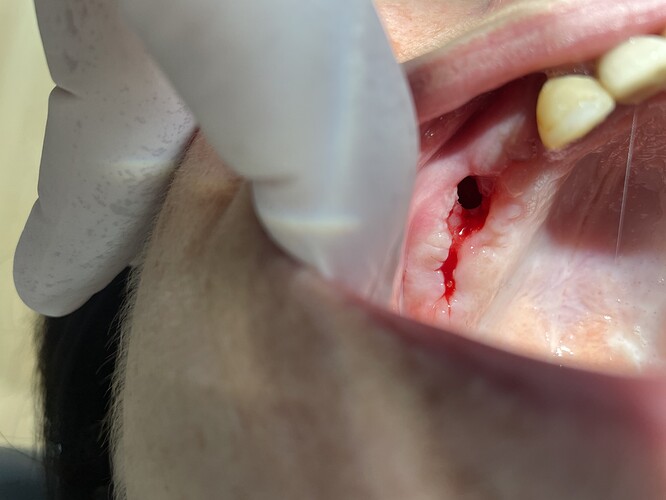
After sinus augmentation the tissues were open. Now there is not enough tissue to close this gap. Any ideas?
John Beckwith DMD DABOI comments:
Dr bOleg Amayev comments:
I understand that you did internal sinus lift and you perforated the sinus and the area not closing. What you need to do is to curet the area to cause bleeding then releasing incision this way you can obtain more than enough tissue to achieve primary closure. When you do this you need to apply mattress sutures. The number one goal is to achieve blood clot.Another way is open the flap, place resorebabel membrane over perforation and follow with releasing incision, etc…
Russe Philippe comments:
How can you start a surgery when you don’t know how to cope with complications, release a flap….. Have you been to a course? Participated to hands-on? What would you answer if you were sued? That you looked at a video on Vumedi or Utube with no scientific commitee Wheeler you can find some of the most ridicule us surgeries, neglecting all the litterature? Extremely sad but very common nowadays P. RusseJohn Townend comments:
It looks as though you have created an oro-antral communication (OAC). Have you performed a Valsava manoeuvre to check for antro-oral air escape? Does the patient report oro-nasal fluid escape? If so it needs surgical closure as soon as possible. There are various techniques but a standard buccal advancement flap - a so-called Rehrmann flap - would be the simplest approach. If you don't know how to close an OAC please refer to an oral surgeon a.s.a.p. Don't try to close it yourself and refer it to an OS when it all falls apart again.Narkhede DDS, MDS comments:
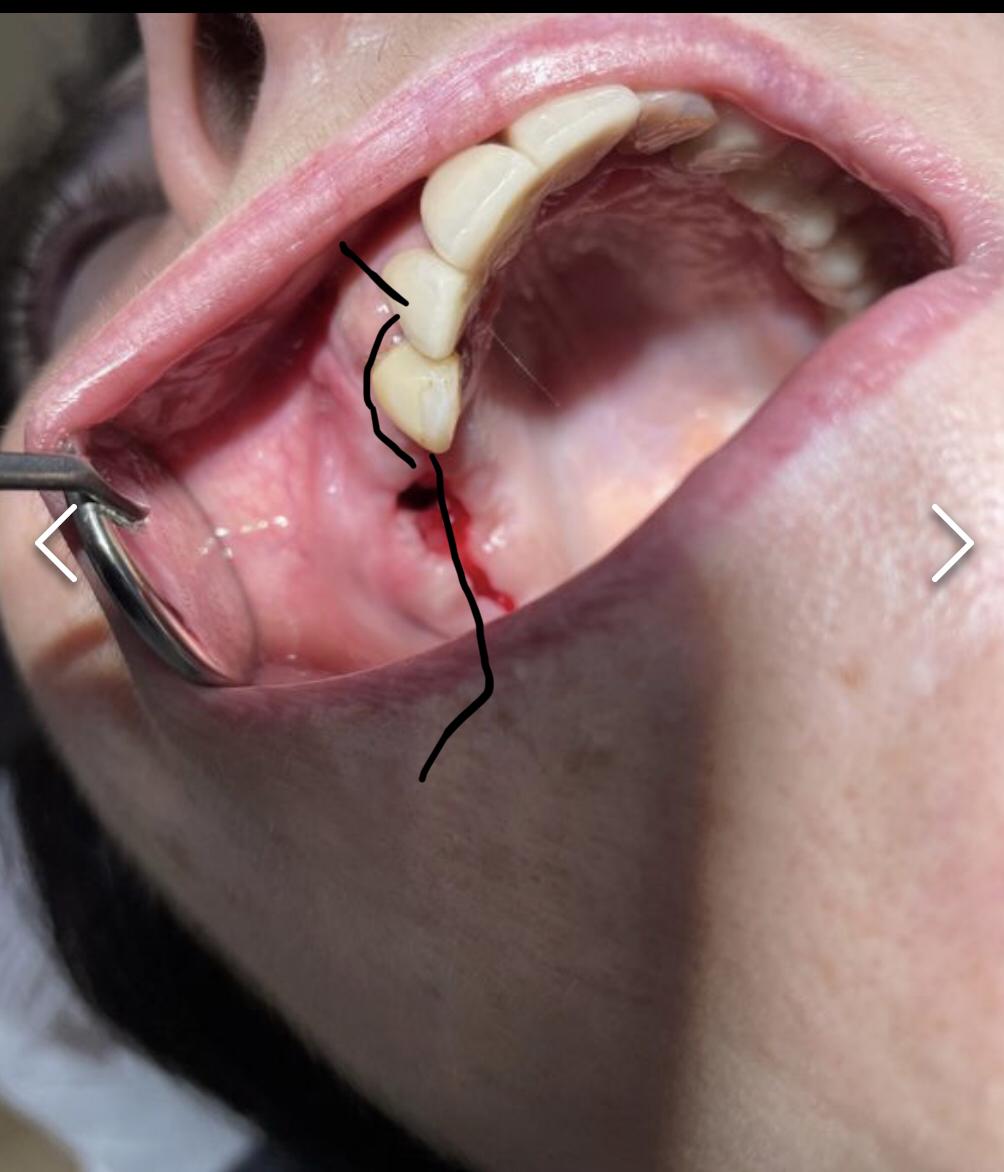Plz ck uploaded image. Make an incision accordingly. Elevate the flap. Release the flap for primary closure. Place membrane over the exposed area. And close with appropriate suturing technique. Hope this helps.
Most of us learn with failures ![]()
Dr. Jennifer Watters comments:
So much can be done with adequate flap design. I’d use PRF also to close communication.Dr John M. comments:
Oh boy!We all need to learn, but to be caught (in this very basic situation) unable to close a flap is concerning. Is the patient still in the chair waiting to find out what advice you got online?
You really do need a little more education prior to lifting that scalpel.
Tasos Dentist comments:
Dr John M , I am doing this since 2005.The reason I upload this case is to get some ideas and not to be critisized by someone I do not even know.I have done all by the protocol but I stuck in this situation.Therefore I tried an advance flap or mattress sutures but I got this again.I think that the reason of this is the buccal loss of bone .Tim Carter comments:
I understand that you are seeking help but to assume that an OA communication is the result of "loss of buccal bone" is really concerning... I am not saying this to be critical. This should be a reminder to all of us on this forum, myself included, that it is ok to refer as we don't need to be "Super Dentist".Dennis Flanagan DDS MSc comments:
buccal fat pad pedicle graftDennis Flanagan DDS MSc comments:
Cut periosteum or place dermal allograft or buccal fat pad graftDennis Flanagan DDS MSc comments:
Cut periosteum or place dermal allograft or buccal fat pad graftDan comments:
Hello everyone First of all this guy is seeking help over here and not be criticized or crucified, The nerds who posted negative post never gave any advice on how to help with the situation, your presence in this platform is useless and unnecessaryTo go back to the main issue
You have what we call OAC ( oro-antral communication) , two ways to approach it
1- advanced buccal flap , one doctor has illustrated it with a post previously
2-palatal pediculated flap where you rotate a flap from the palate and cover the communication
Place the patient on antibiotics/ antihistamine accordingly and follow up
Good luck Doc
THOSE WHO NEVER MAKE MISTAKES, NEVER WORKS ENOUGH!
Manosteel comments:
My thoughts exactly!Jerry Schwartz comments:
Consider this...surgical approach with advancing flap will work; however, this is much simpler....curette, establish significant bleeding, place mixture of Calcium sulfate and Tetracycline, and place cyanoacrylate on top of this and wound edges....almost guaranteed to work...the fibroblasts love the calcium sulfate and cyanoacrylate...should see rapid epithelialization and healing....good luck!Matt Helm DDS comments:
The gold standard for closing an OAC is to suture the Schneiderian membrane tear. All other solutions, while viable in some cases, are second-best. That's not to say they won't work, just that they can be unpredictable. IMHO, referral to an OS would best serve the patient's best interest long term, as well as yours. If you're in the US, you may have to answer to a lawsuit and, if you're a GP and did not refer to an OS, that's about the worst thing you can do. Mistakes and accidents happen to all. However, how you handle them is crucial. I don't know the extent of your general surgical training or expertise, but my instinct tells me that if you had to come on here to ask for advice, you don't have the experience to advance a palatal pedicle flap, or perform any of the other suggestions given -- all valid, but not always free of complications. Do the right thing and refer the patient to a good Oral Surgeon ASAP. An active, open OAC must be closed as soon as possible, or the infectious complications can take a long time to heal. Your patient will thank you, your peace of mind will thank you and, most of all, your career will thank you. We can all run into difficulty, but it's knowing when to back off and refer to the specialist that makes the ultimate difference. "Don't try to be a hero" are golden words.Dr D. comments:
Colleague, from this description and from the picture, do not understand how the condition of the sinusitis is before and after the intervention. Whether the process is active before or now the solution is different. Show the x-ray!Richard Benian comments:
Could you please give more detail of your case? This is not a difficult situation to treat, but it would be helpful if you gave more information. Thank you.Tim Carter comments:
I actually had a very similar case referred to me recently and what I ultimately did which solved the problem was quite simple. Make a crestal incision to allow an elevator in to release the buccal and palatal tissue. Place a collagen wound dressing (Colla Cote/Colla Tape etc...) over the perforation to stabilize a clot and then cover that with a PTFE membrane. Suture with whatever material you desire and after 3-4 weeks you can simply remove the PTFE and you should discover a nice epithelial lining perfect for continued healing and maturation. Or you could refer...