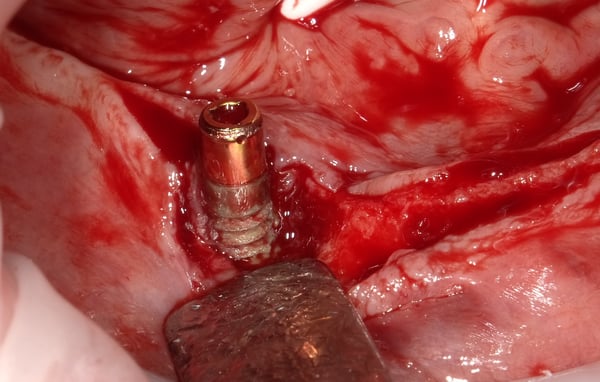
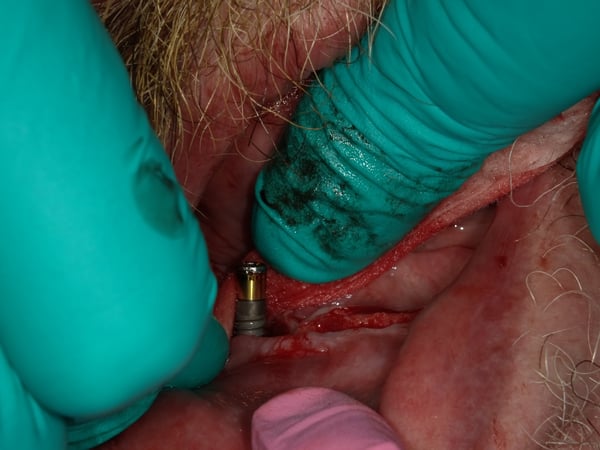
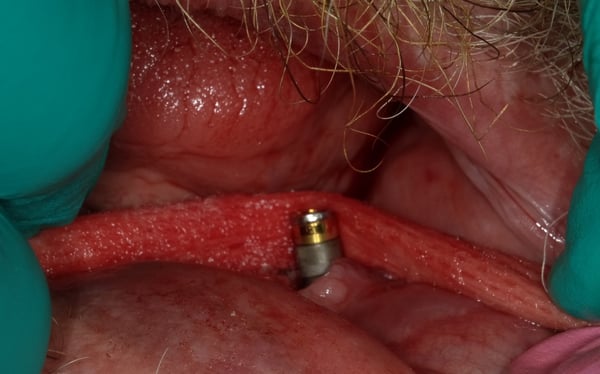
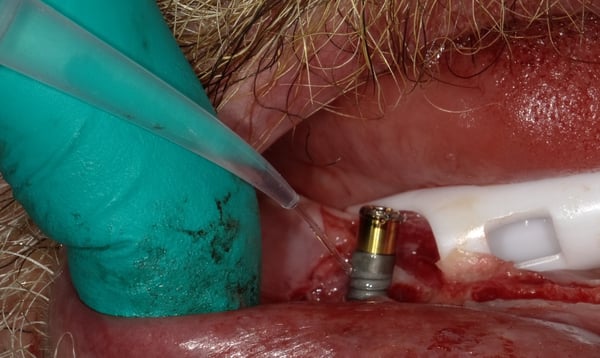
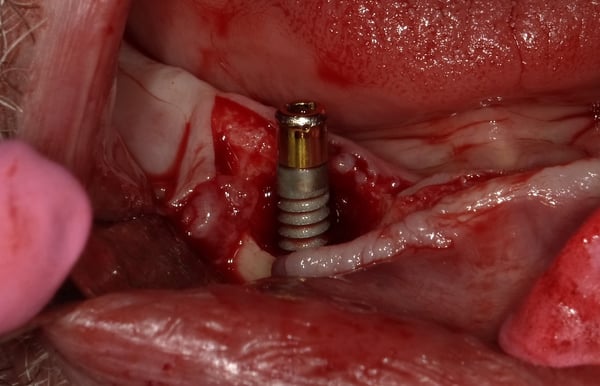
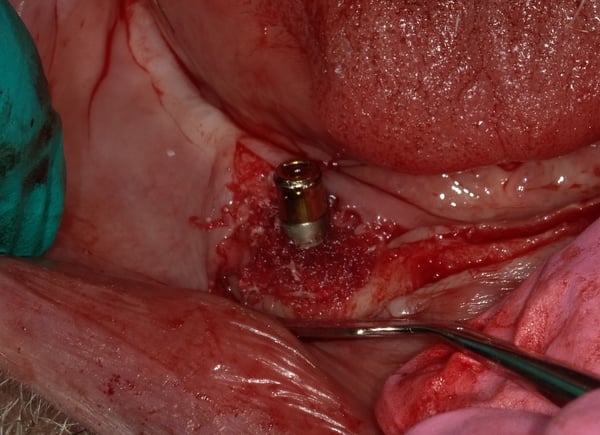
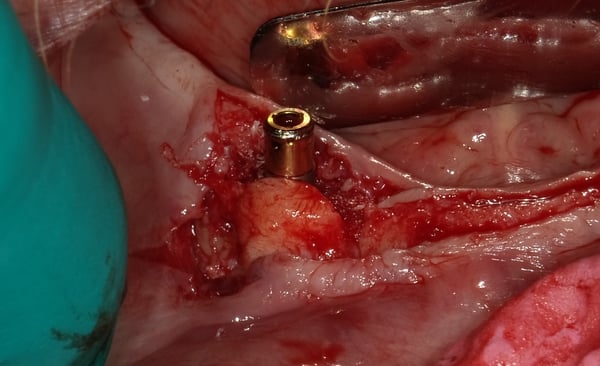
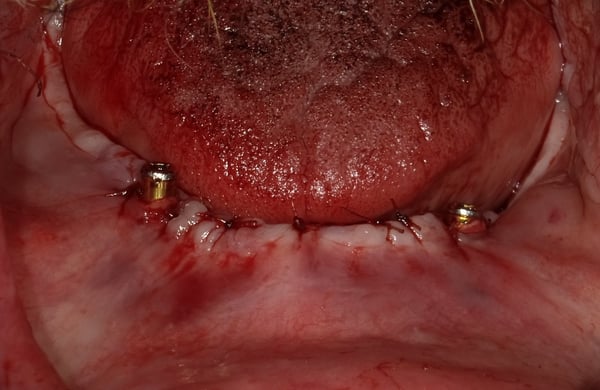
During my perio residency 2004-2007 we were taught to treat peri-implant defects as though they were teeth, which they are not. We used plastic and/or titanium instruments and often resorted to plasty of the implant threads.... The end result was cross your fingers and hope for a miracle. Recent studies, and my own clinical experience, has demonstrated that scrubbing and rinsing with sterile water should be the only instrument, other than an end tufted brush to contact the surface. Attached is a case demonstrating the treatment of peri-implantitis...
smartzookie comments:
I treat it with an open flap and the use of ER:yag and Ozone, sticky bone and PRF sometimes collagen and PRF membranes. Works better than “old school”. I don’t treat this closed flap unless very minor
Bone loss because I need access to the threads to clean individually with the laser.
timcarter comments:
I have used ER: yag and Nd:yag and both have demonstrated variable results most likely attributed to the disruption of the oxidative layer on the fixture surface. The overwhelming majority of the non biased/non manufacturer funded research suggest copious irrigation with sterile water as the treatment of choice... This has been a paradigm shift for me as well since I too like to utilize my toys!!
sboms comments:
A couple of thoughts:
1. I would have buried this with a water tight primary closure. With the locator abutment in place, it will act as a tunnel for saliva and bacteria to get pumped into your wound from the denture. Relieve the denture so minimal pressure on the site. No denture adhesive. Uncover after 16-20 weeks. When you uncover, you can bring more keratized tissue to the facial aspect. The patient won't like it, but that's how it goes with a two implant retained over denture. You put a a lot of time and effort into this procedure, but I think your jugular is exposed with the transmucosal healing.
2. 20 years in and I do my best to do as few of these cases as possible. My highest implant failure rate is in my removable cases. Fixed, while more expensive, is much more dependable in the long run. I happen to practice in an area where most patients can afford it, so I've been lucky I guess. I do, however, spend a lot of time with my full arch consults and take the time to show them what's possible. Maybe let this patient know that a future upgrade is possible. Show them models of what a fixed case looks like vs. removable. Let them think about it for a while, and they may come back and ask you for the upgrade. At that point you've already got a great temporary that can be converted to a fixed hybrid.
wiseox comments:
I'm taking the question literally; I'd use rotary wire debridement brushes, scrub/irrigate with diluted NaOH2, graft, remove Locator, nice water-tight sutures. Get them on a triclosan toothpaste. I like to do frequent checks during healing to reinforce OH.
timcarter comments:
Why triclosan toothpaste?? I used rotary titanium wire brushes for years but recent data suggests tat it might be a poor choice. The abrasive metal, even though it is titanium, destroys the oxidative layer and seems to lead to worse outcomes. and while not mentioned it has also been suggested to avoid CHX/Peridex at all costs...
gregkammeyer comments:
I use titanium currettes, then wire brush, and gylcerine air abrasion. I believe I'll be doing more implanotoplasty after reading a recent Meta_anlaisis.
timcarter comments:
It is nice to see people actually respond to a post in the manner intended. I am in no way stating that the case I posted here is properly done and am hoping to hear from others on how they handle peri-implantitis.
wiseox comments:
Tell us about the Meta Analysis Greg.
timcarter comments:
I would like to know more about the use of triclosan toothpaste. I have read that diluted NaOH2 is good as long as the dilution is at least 5:1 (water:5% bleach) solution. Because the bleach is toxic in higher concentrations it is recommended to use plain sterile water.







