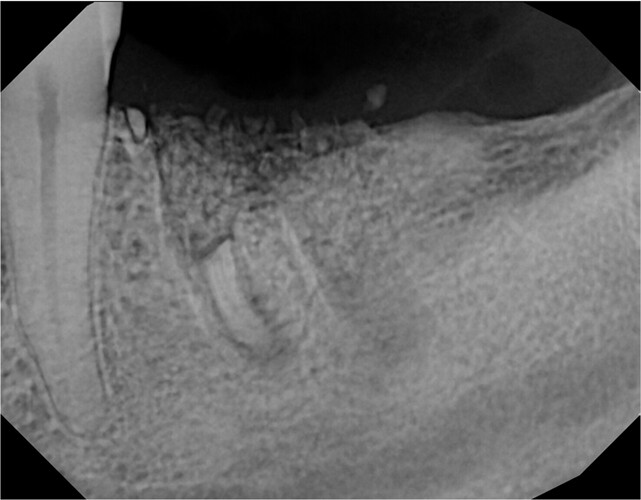
Tooth #19 was extracted 2 weeks ago and the socket was preserved with the placement of a bone graft and membrane. The patient continued to report pain that was not improving over time and a second opinion was consulted. A periapical radiograph was taken and it was noticed that the apex of the mesial root was still present. The tooth likely fractured during extraction and was removed in pieces. Failure to confirm complete removal of the entire tooth resulted in missing this root apex. Unfortunately, the graft and membrane had to be removed and the root apex was identified and extracted. Whenever we encounter a complicated extraction where the tooth is removed in pieces, we should adapt the habit of confirming COMPLETE removal of the tooth with a post-extraction radiograph before proceeding with any further treatment. How do you approach a complicated extraction? How do you ensure complete removal of all tooth remnants?
I would completely remove the buccal plate to get access for removing this via a buccal approach. The removal of the buccal plate does not concern me as it will leave a 3 walled contained defect which is an ideal situation for receiving a graft even without the addition of a membrane. I suspect that the buccal pate is completely intact here or else the root tip would have been detected and removed. I do not graft intact posterior sites and in this case I would most likely have opted to place the implant immediately after removing the root tip… It is always my preference to place the fixture at the time of extraction when possible.
Obviously , examine extracted roots prior to grafting.
I tell all my students and residents
…stay within your lane. If you dont have experience w surgical extractions, please refer it out.Saves you time, aggravation and legal issues
Try using surgical piezo to remove root tips without removing any walls. Surgical mallet helps. Avoid destruction of socket walls. Be gentle- tissues heal better
The goal is not to remove the buccal plate and hence not have to restore it.
Removal of some of the intraseptal bone in this situation is the answer.
After the intraseptal bone is removed , a small baby cryer of curved root tip pick can remove the remnan up vertically through the socket. The intraseptal bone will come back providing the 4 walls of the socket remain intact.
First thing to do is to take a break, step out of the room, breathe and then come back. Take a radiographic and proceed with removing interseptal bone.
This is a situation where using a straight attachment handpiece is a better call VS a surgical highspeed for access purposes. Sometimes, the surgical high-speed can touch the adjacent teeth making accessibility is often challenging.
Also, ensure adequate suction and dryness of the surgical field from blood and debris as much possible to ensure visibility. It happened to me few years ago. I learned the hard way. Piezo is a great option too if its available.
I agree completely with this. My old OS instructor used to say “Make room to get the damn thing out, You need access to be successful.” BTW that was 40 years before we had the grafting techniques and surgical forceps like a physics forcep.
Only Two things are needed to remove a broken root tip
1.Small 2mm suction tip
2.Headlamp
And patience!!
That’s it!!
All great suggestions, I would relate when I’ve had diff root tips, I dig out either my Zeiss Loupes, with illumination. They may be cumberson, I also have Sun system set up as well. But what a difference it makes when you’re trying to finesse out a F’n pesky root tip! Sometimes you got to make more of a flap for visual purposes, but I would leave the buccal approach for last resort. Root tip Picks, Periotomes, Patience (the 3 Ps lol)
One general assumption I am going to make based on my experience is that this patient most likely has a thick buccal plate and thus an abundance of thick keratinized soft tissue covering the buccal. I am making this assumption based off the fact that this rather large root tip is retained following the partial removal of a relatively short rooted molar with a wide area of seemingly vascular cancellous septal bone. If not for the thickness of the existing buccal plate of bone this fragment would have most likely rolled out to the buccal during the luxation. Given all of this I believe that if indeed an implant fixture is planned for this site then the first step is to completely remove the root. In this case it seems to have been predetermined that some sort of a particulate graft would be “needed” so a commitment has been made to preserve/restore regardless of the condition of the remaining buccal plate. Thick existing buccal bone + thick overlying keratinized soft tissue + thick and porous septal area = feel free to remove a portion of the buccal plate to gain access for removal and rest assured that this remaining 3 walled defect will heal. I have also come to believe that many of our efforts to perform “atraumatic” extractions in an effort to preserve this poorly vascularized holy grail of a buccal plate can often lead to more damage due to heat and compression from trying to slip tiny little instruments into tight spaced to address these cases. Bottom line, you can most likely address this any any of a number of methods but in my opinion most of the fancy, made for publication techniques, do not apply to this mandibular posterior site that most likely has sufficient attached keratinized gingiva to allow nothing short of murder to be successful…
This jab is unnecessary and flippant. You can easily state your opinion, without insulting or demeaning others hard work. It would actually give your comments more credence. Thank you.
The issue is that this individual clearly made a predetermination to “restore” this site with a graft so all of the effort to preserve the plate is null and void. It is more important to completely remove the root and a well preserved extraction site should not require a graft for proper healing. Either you commit to preservation or you commit to grafting and a 3 walled posterior grafted extraction site will heal extremely well. This is just my opinion/observation and do not claim to have the answers only to call into question claims that do not make sense to me…
My apologies to anyone whom I may have offended with my poor choice of words to describe this particular situation. My intention was never to criticize anyone and if I offended you please accept my apology and may we continue to discuss and learn.
Vision, access and a path of removal. The interseptal bone was clearly not removed nor the root tips examined nor the socket examined to confirm complete tooth removal. These 2 lines are my bottom line.
Yes, a PO x-ray would confirm that. LOOPS and a HEAD LIGHT are essential as is control of the bleeding. Both keeping and removing the Buccal plate are acceptable. Certainly EZ to grow the plate back.
Three things I would like to discuss with the contributing member regarding this particular case:
1: Why is it so important to preserve the buccal plate on this mandibular molar?
2. Why sacrifice the porous/cancellous septal bone in order to preserve less vascular buccal plate?
3. Why do you graft a fully intact posterior socket?
A more zebra approach would be (always take a post op PA when unsure of complete removal), gut out the interradicular bone with a trough by a long bur (there’s an undercut on the distal wall of this root), get around the mesial side of the root with a piezo tip which you can take a pa of it in position, then take an east west or cryer and deliver the root tip, graft the socket with 30/70 corticocancellous bone and let heal 5-6 months. There’s also a tooth frag distal to the premolar to tease out as well.